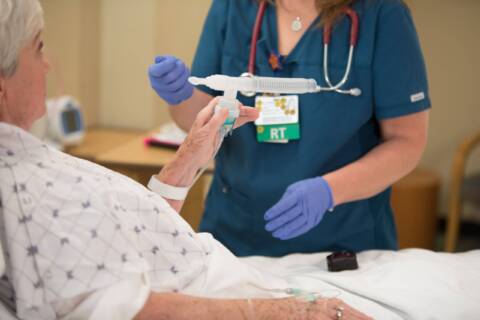
Respiratory Therapists Collaborate with Healthcare Professionals for Patient Care
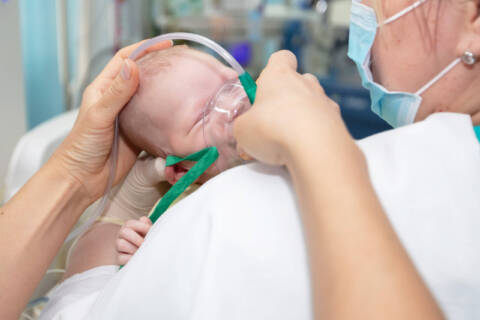
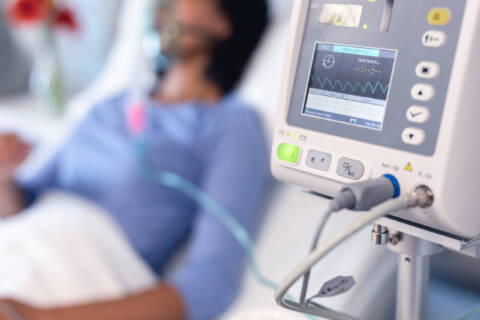
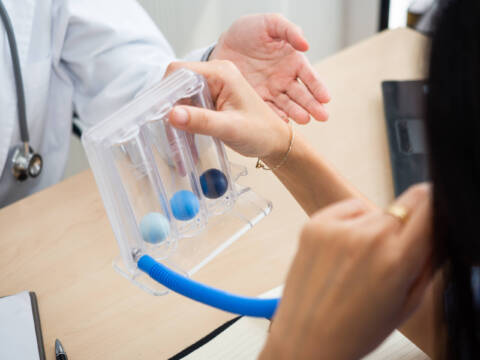
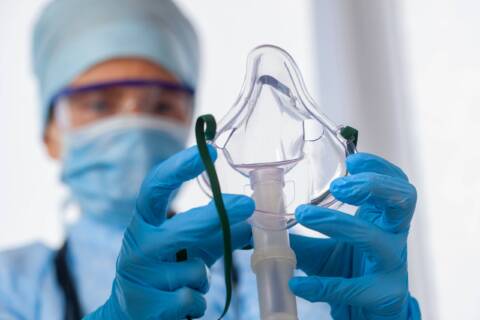
A diagnosis is just the beginning of a long journey toward treatment and improvement. Along the way, patients receive comprehensive treatment from a myriad of healthcare professionals who all work together to restore their health and well-being. Respiratory therapists (RTs) are key healthcare professionals in this process, often participating in treatment, like performing pulmonary function tests or operating ventilators, at multiple steps along the way. In a clinical setting, respiratory therapists help patients manage their breathing problems with evidence-based techniques. In an allergy and asthma clinic, they may be performing the diagnosis themselves, but they can also help develop treatment plans for patients who have been diagnosed by primary care physicians or other healthcare specialists. Interdisciplinary rounds are an integral part of multidisciplinary care. Various healthcare professionals examine patients together to develop a comprehensive care plan that incorporates multiple fields into one treatment plan. By combining expertise and working together, healthcare professionals can enhance their patient’s quality of care from all angles. During interdisciplinary rounds, respiratory therapists may provide updates on the patient’s respiratory status, including lung function, oxygenation and ventilation. RTs are equipped to provide insights into the patient’s ability to maintain a patent (unobstructed) airway and advise on interventions to address any airway-related issues with physicians, nurses, pulmonologists and other healthcare professionals. By contributing their expertise in respiratory care, they can help develop and implement an effective, integrated care plan. RTs are responsible for ensuring the patient’s ventilator support equipment, chest physiotherapy equipment and airway management tools are working properly. This may include management of a variety of devices, from simple nasal cannulas to more complex devices such as capnographs and nebulizers. You can learn more about which medical devices respiratory therapists are responsible for in our blog on the topic . Respiratory therapists and pulmonologists frequently work together to curate a personalized, effective treatment for patients with breathing problems. While they share a similar focus, the two professions have a unique set of duties. Put simply, pulmonologists are doctors who focus on diagnosing and developing treatment plans, while respiratory therapists come after in the treatment pipeline with a focus on providing the therapies, managing symptoms and educating patients about breathing devices and exercises. Pulmonologists are primarily utilized in complex cases, while respiratory therapists work with a range of breathing conditions that vary in severity. Moreover, because the conditions pulmonologists see are more serious in nature, they are usually confined to internal medicine departments in hospitals. Although respiratory therapists are most often employed in hospital and critical care settings, the role has recently expanded into as well as clinics and community health centers. Most respiratory therapists work most closely with nurses and pulmonologists, but opportunities are becoming available for collaboration outside of a hospital setting. This can be especially useful if you’re hoping to specialize in home health or geriatric care – specializations St. Louis College of Health Career offers reputable programs for. Respiratory therapy is rapidly growing in demand and job prospects, with the field projected to grow by . At St. Louis College of Health Careers, our respiratory therapy program thoroughly prepares our students, providing the knowledge they need to sit for the NBRC board exam and perform well at their jobs from the get-go. Our RT degree will help you understand how to optimally diagnose, plan and treat patients with breathing problems – as well as how to collaborate with other healthcare professionals effectively to ensure your patients receive high-quality care. Get started with an in-depth yet flexible education by calling 866-529-2070 today to learn more about our .